Voices of Biotech
Podcast: MilliporeSigma says education vital to creating unbreakable chain for sustainability
MilliporeSigma discusses the importance of people, education, and the benefits of embracing discomfort to bolster sustainability efforts.
September 30, 2021
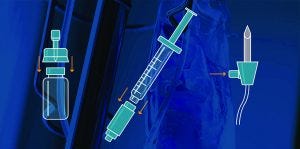
Closed-system transfer devices facilitate preparation and administration of precise
injectable doses. (reference 3)
Ever since the first biopharmaceutical product (biologic) was approved in the 1980s, companies have developed protocols and tests to ensure that such products are safe and effective. Biologics are very different from traditional small-molecule drugs, with unique risks inherent to their manufacturing processes. Biopharmaceutical formulations often present as complex mixtures that can be sensitive to heat, light, and many other factors, all of which must be monitored and assessed. However, until recently, developers worked mostly independently, with only their own resources and expertise to develop those assessments and set acceptable parameters.
BioPhorum recognized that that competing companies could work together and share information in many ways that would accelerate progress for everyone. We identified two areas in which this was especially timely: compatibility assessments of biopharmaceutical products in general and, more specifically, of closed-system drug-transfer devices, which mechanically prevent both transfer of environmental contaminants into a drug formulation and the escape of drug/vapor concentrations outside the system (1). Examples include OnGuard/Tevadaptor technologies from B. Braun Medical, PhaSeal and SmartSite devices from BD Bioscience, and ChemoClave and ChemoLock devices from ICU Medical.
Hazardous Drugs (HDs) |
USP <800> defines hazardous drugs as those identified by at least one of the following criteria:
In a biopharmaceutical context, this designation mostly applies to radioconjugates and antibody–drug conjugates. |
Compatibility Assessment
Those different types of closed-system transfer devices approved for use by the US Food and Drug Administration (FDA) feature a wide range of designs and materials. The use of such devices has increased gradually since their introduction in 1998, but the pace quickened significantly in recent years when both the National Institute for Occupational Safety and Health (NIOSH) and the US Pharmacopeia (USP) started recommending them for the preparation and administration of hazardous drugs (1, 2). Such use has expanded over time to include some biologics, which can have similar indications but very different risk factors from those of other “hazardous” drugs. However, little guidance has been available from regulatory agencies on how to conduct the necessary compatibility assessments for biopharmaceuticals.
The large range of closed-system transfer devices, components, materials, and other confounding factors make comprehensive testing impractical. Until now, each company has worked independently to develop assessment protocols and mitigate risks. A recently published, peer-reviewed journal article — the results of an 18-month collaboration among industry experts on the topic of CTSD compatibility assessment — has changed that (3).
Ligi Mathews (principal pharmacist at Janssen Research and Development) explains: “There was a lot of ambiguity in the industry. This collaboration brought clarity and provided some best practices for assessing the risks for each closed-system transfer device. My company already has benefited from the clarity that this information has provided. It has enhanced our ability to derisk [closed-system transfer-device choices] and adopt a more systematic approach.”
Closed-system transfer-device compatibility concerns include materials of construction, formulation concentration ranges, and storage times and conditions (3). In addition to testing those, developers often perform simulated in-use testing both before and after storage using representative equipment/devices. Product quality attributes are assessed to monitor physical and chemical instabilities and protein adsorption over time, typically focusing on visible and subvisible particles; formulation clarity/opalescence, color, and pH; and protein concentration, purity, and potency.
The paper arose from extensive discussions among members of BioPhorum’s formulation workstream, including 16 experts sharing the experiences of their 10 different companies. The group distilled all that knowledge into a single document, which includes a summary of possible patient-safety risks and mitigation strategies stemming from the use of closed-system transfer devices and provides a decision tree for risk assessment of closed-system transfer-device compatibility. Its publication should help biopharmaceutical developers compare their practices with current industry standards. The publication already is having an effect. Kevin Muthurania (associate director of Janssen Research and Development) says that it “opens up a new, wider perspective on our thinking and gets us out of our cocoons. You don’t find a lot of papers on clinical in-use administration, which is a complex area with many different modalities. This work allows us to [identify] what has been a problem elsewhere, and how it was resolved, thus improving our efficiency and validating our own concerns and conclusions. There is extra value for those who are members of BioPhorum and participate in the discussion. We understand the context and more of the reasons behind the specific recommendations.”
“This is especially valuable for academic institutions and smaller pharmaceutical companies that don’t have as many resources,” adds Douglas Kamen (associate director of formulation development at Regeneron Pharmaceuticals).
In-Use Stability
Although providing detailed methods for assessing closed-system transfer devices is useful, the formulation workstream members also had realized that developers sorely needed a broader look at in-use stability studies across the biopharmaceutical industry. Companies expressed a strong desire to explore and benchmark current best practices in both clinical and nonclinical laboratory studies. That would include identifying and quantifying factors that might affect the identity, strength, quality, purity, or potency of biological products, especially as those relate to safety and effectiveness.
The resulting work produced a paper on compatibility and in-use stability studies to enable administration of biopharmaceutical drug products (4). It details specific responses to five separate benchmarking surveys that were sent to 16 companies, and it has been submitted for publication in a peer-reviewed journal. Between 10 and 13 companies responded to each survey, providing a good overview of current industry practices. The surveys covered regulatory strategies and feedback; clinical in-use formulation, patient, and site considerations; clinical blinding, masking and placebo approaches; study setup, execution, and reporting; and clinical and in-use stability testing to provide a comprehensive picture of the range of common industry practices.”
“What we learned is that there is no single guidance,” says Charavarthy Narasimhan (senior principal scientist at Merck), “but instead there are multiple ways to conduct these studies, and regulatory bodies are accepting a variety of methods. This diversity of approaches means that there is clear need to propagate this information to pharmaceutical companies, so they can develop robust injectable products.”
George Crotts (a director at GlaxoSmithKline) elaborates: “The diversity in approaches is not a bad thing. This group of authors has identified the allowable variability and flexibility in approaches, while at the same time providing insight for the boundaries on times, volumes, temperatures and other parameters utilized across the industry. This cross-company collaboration is an excellent way to significantly [improve] product quality.”
Kamen says that the questions “were developed by the authors, who are researchers in the field and wanted the answers for themselves. They developed a set of practices that work, but not a single set of best practices. Because all these methods work, you can select what is best for the particular needs of your own company’s clinical program.”
For Patients and Providers Alike
These two latest publications together provide a comprehensive overview of the state of the art in compatibility testing and in-use stability studies for biopharmaceutical drug products. By making this information publicly available, the authors have enabled groups across the industry to leverage what others have learned rather than starting from scratch themselves. That should help each organization use its own resources more efficiently and effectively while developing strategies based on real-world experience for continuous improvement and innovation through their own assessments.
By working together and sharing information, companies can develop better tests for their own products. These efforts ultimately will help to ensure that patients receive safe and efficacious biologics and that healthcare workers are protected, providing the best possible public health outcomes for all.
References
1 Preventing Occupational Exposure to Antineoplastic and Other Hazardous Drugs in Health Care Settings. National Institute for Occupational Safety and Health (NIOSH): Washington, DC, September 2004: https://www.cdc.gov/niosh/docs/2004-165.
2 <800> Hazardous Drugs: Handling in Healthcare Settings. USP 40–NF 35, 1 July 2018.
3 Besheer A, et al. An Industry Perspective on Compatibility Assessment of Closed System Drug-Transfer Devices for Biologics. J. Pharm. Sci. 110(2) 2021: 610–614; https://doi.org/10.1016/j.xphs.2020.10.047.
4 Stokes E, et al. An Intercompany Perspective on Compatibility and In-Use Stability Studies to Enable Administration of Biopharmaceutical Drug Products. J. Pharm. Sci. 2021: submitted.
Further Reading
Morar-Mitrica S, et al. An Intercompany Perspective
on Biopharmaceutical Drug Product Robustness Studies. J. Pharm. Sci. 107(2) 2018: 529–542; https://doi.org/10.1016/j.xphs.2017.10.017.
Scott C, Ritter N. Stability Testing: Monitoring Biological Product Quality Over Time. BioProcess Int. 19(3) 2021: https://bioprocessintl.com/analytical/qa-qc/stability-testing-monitoring-biological-product-quality-over-time.
Scott C, Gazaille B. Formulation, Fill–Finish — Biopharmaceutical Drug-Product Trends and Technologies. BioProcess Int. eBook 29 January 2021; https://bioprocessintl.com/manufacturing/fill-finish/ebook-formulation-fill-finish-biopharmaceutical-drug-product-manufacturing-trends-and-technologies.
Elaine S. E. Stokes is an account manager and facilitator
at BioPhorum based in the United Kingdom; [email protected].
You May Also Like